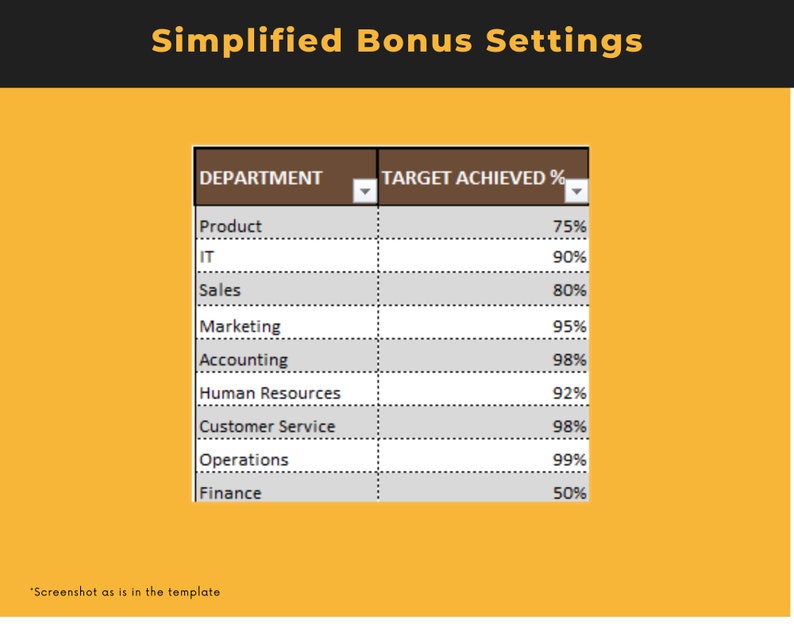
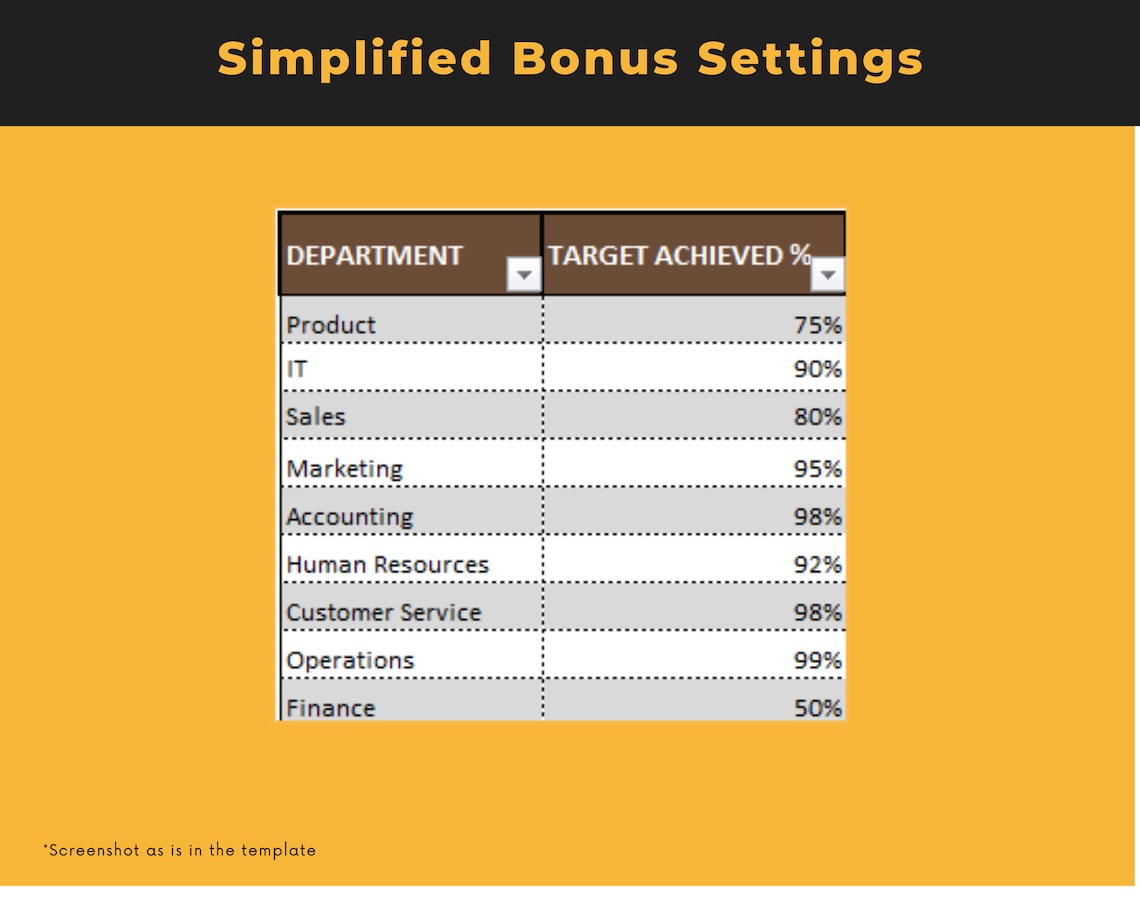
Price:TOKO22: Situs Slot Gacor Bet 400 Gampang Menang Terpercaya Se Indonesia
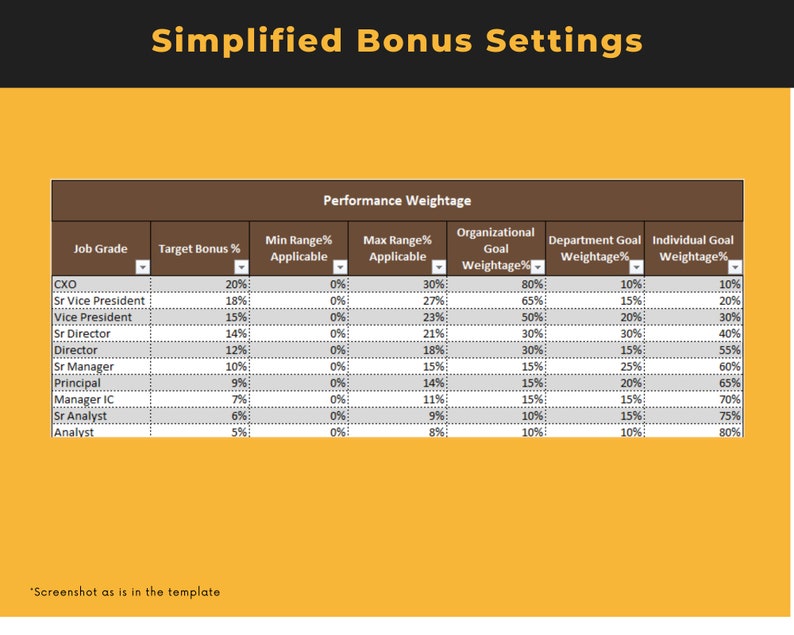
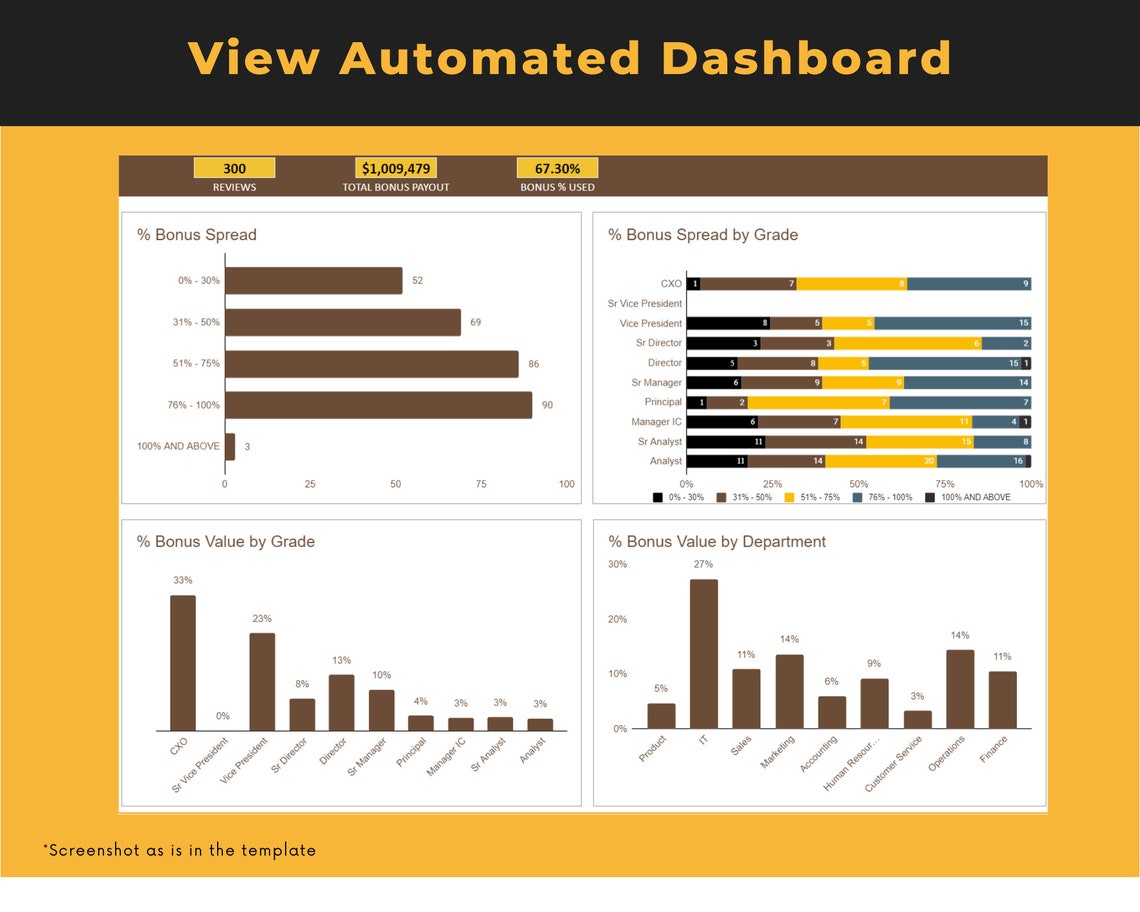
TOKO22 hadir sebagai link resmi terbaru yang paling dinanti. Situs ini secara khusus menghadirkan koleksi game Slot777 dan Slot88 yang sedang dalam kondisi "gacor" terbaik, didukung server khusus yang menjamin kenyamanan dan peluang maxwin tertinggi. Dengan server Slot777 dan Slot88 resmi yang stabil dan gacor, TOKO22 menghadirkan pengalaman bermain lancar, bonus melimpah, serta peluang maxwin tinggi di setiap putaran. Bergabunglah sekarang di TOKO22, nikmati permainan seru, RTP tinggi, dan buktikan sendiri hoki malam ini hanya di situs slot resmi paling gacor tahun 2025!
You can only make an offer when buying a single item
Highlights
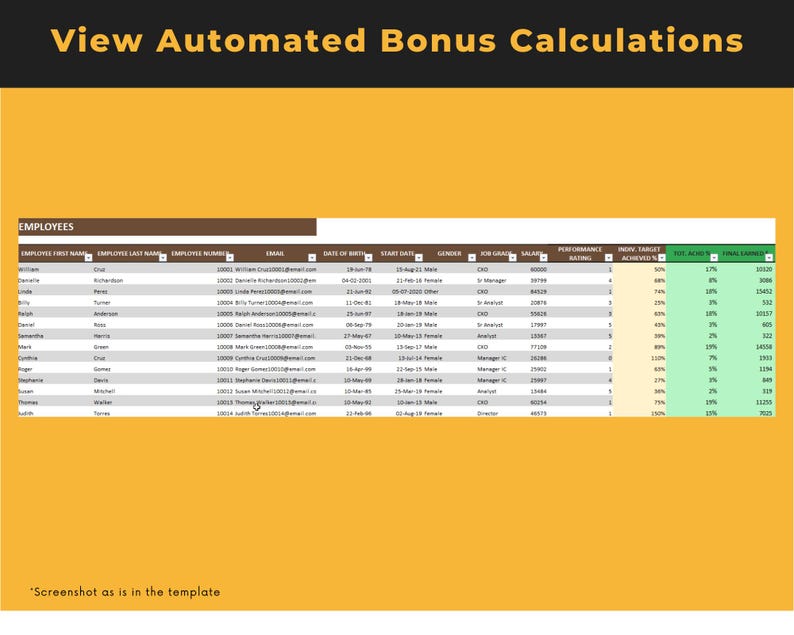
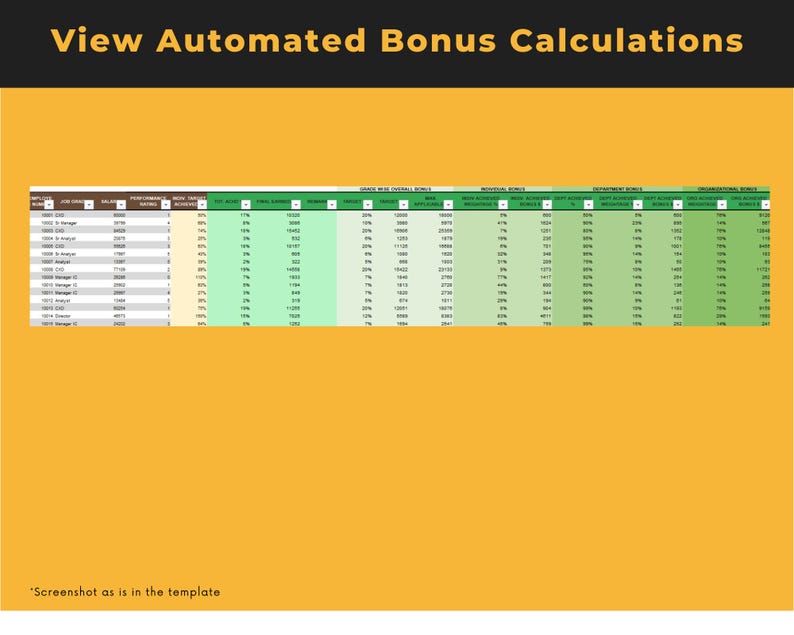
TOKO22 adalah situs slot gacor paling resmi dan terpercaya se indonesia mudah menang bocoran RTP akurat winrate 98% , bet 400 mindepo 10K sudah bisa langsung dengan cepat mendapatkan kemenangan luar biasa , layanan 24 jam deposit via QRIS sangat cepat memudahkan player langsung dapat bermain dan mendapatkan kemenangan, gabung sekarang juga di TOKO22.
4.9 out of 5
(618 reviews)
All reviews are from verified buyers
Reviews for this shop
Daftar dan langsung dapet maxwin besar di TOKO22! Seru banget!
Ini situs TOKO22 seru banget! Sekali deposit langsung dapat jackpot gede!
Di TOKO22 deposit sudah murah hanya 10rb dan bisa main semua slot lagi!.